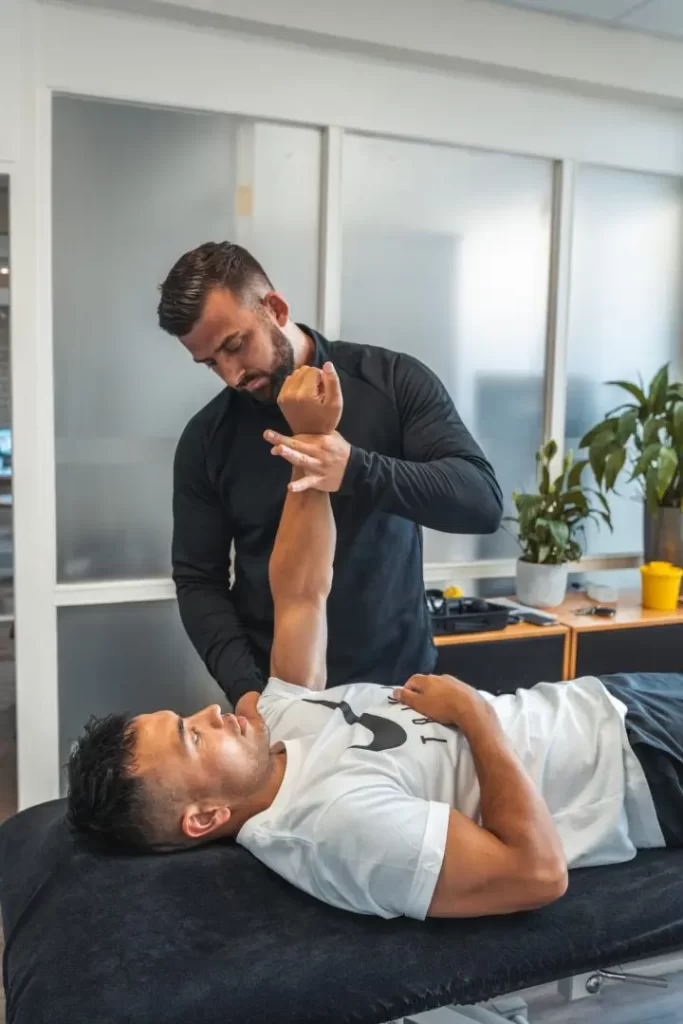
Frozen shoulder
Frozen shoulder, also called frozen shoulder or adhesive capsulitis, is a condition of the shoulder in which there is pain along with limited range of motion of the shoulder. This may limit you in your daily life. For example, the reduced mobility in the shoulder can make it difficult to comb your hair, grab something from your back pocket or grasp anything above shoulder height. The pain can also cause problems with sleeping.
A frozen shoulder is a 'self-limiting disease'. This means that the disease process may go away on its own. Depending on recovery impeding factors, the total duration of the condition can vary from 4 months to 3 years or sometimes more

Cause
The cause of a frozen shoulder is often not clear. What we do know is that a frozen shoulder is more likely to occur if it has been preceded by surgery or a moment of trauma (i.e. a fall or collision). Also, people with diabetes, for example, or in people with an autoimmune disorder have a higher chance of developing a frozen shoulder. It is more common in women than in men and in people aged between 40 and 59.
Common symptoms in frozen shoulder pain when lying on the shoulder
- pain when lifting the arm
- pain when turning the arm outwards with the elbow in the side
- Sometimes there is radiation in the upper arm
- Quick and unexpected movements cause pain
Physical examination for a frozen shoulder
If we recognise with during the history a recognisable pattern as in frozen shoulder, we are going to do some tests. There is no specific test to diagnose frozen shoulder. In practice, we test the active and passive movement in the shoulder. Together with the recognisable symptoms and course of the complaint then a suspicion can be expressed about the diagnosis of frozen shoulder.
The treatment for a frozen shoulder
The treatment of a frozen shoulder consists of several aspects. Initially, we opt for pain relief through massage. Next, we look at the range of motion in the shoulder and tackle it in a targeted way through mobilising exercises in the room and exercise room. During treatment, we take into account the reactivity of the shoulder along with its phase. At the beginning of the treatment period, the emphasis is on relatively pain-free exercises to increase or maintain mobility. At a later stage, it is necessary to optimise the entire chain of motion of the shoulder girdle, and more active exercises are performed towards all end positions. Sometimes a corticosteroid injection may be chosen. Especially in the early stages, this can provide relief from symptoms. In later stages, it has little or no added value. Other pain relief may possibly provide some relief and provide some rest between treatments.
The quick facts
- Women are more likely to have frozen shoulder than men
- In the 40-59 age group, frozen shoulder is most common
- People with an autoimmune disease or diabetes are more likely to develop a frozen shoulder
- Sometimes a frozen shoulder occurs as a result of a fall or surgery
- A frozen shoulder is a self-limiting disease, meaning symptoms will eventually disappear without intervention really being necessary
- The condition can last from 4 months to 3 years
Stages
Phase 1: also called freezing phase or painful phase. In this phase, there is mainly pain in the shoulder.
Phase 2: also called frozen phase or stiff phase. In this phase, there is less pain, but the mobility of the shoulder has deteriorated a lot.
Phase 3: also called thawning phase. In this phase, the shoulder ''thaws out''. The pain decreases further and mobility will gradually increase again.
Making an appointment at FysioFitaal
We work from multiple locations in Tilburg, always close by for professional and accessible physiotherapy. Fill in the contact form and we will contact you soon. Together, we will work on your recovery!