Proximal hamstring complaints
Proximal hamstring injuries are injuries that occur at the level of the attachment of the hamstring to the ischium. In medical jargon, this is also called the tuber ischiadium. This injury is common in athletes after an explosive movement. Think of a sprint. But also an overstretching with, for example, gymnastics, martial arts or a footballer just trying to retrieve a ball in an extreme attempt. We then call this a stretch type. In addition, non-athletes can also develop complaints from prolonged sitting or a sudden overuse of the hamstring region. The symptoms are located in the buttock region and can radiate down the back of the thigh.

Causes for proximal hamstring complaints
Proximal hamstring injury can occur in several ways. Acute overstretching occurs during a sudden and powerful movement, such as when starting a sprint or making a high kick. Long-term overuse is another cause and occurs when the tendons are under stress for a long time without sufficient recovery time, such as in long-distance runners.
Sprint type hamstring injury
Research shows that a sprint-type hamstring injury often occurs in the final phase of the swing movement during running. In this phase, the hamstrings come on stretch while also having to tighten hard. This happens just before the foot hits the ground. Since there is no contact with the ground in sprinting during this phase, the hamstrings absorb these forces. The faster a person can run, the greater the strain. This also increases the risk of a hamstring injury.
Stretch type hamstring injury
This injury results from a quick, larger stretch on the hamstring. Think of a gymnast or a martial artist with a high kick. This injury is most common in sports such as dancing, martial arts, gymnastics and water skiing. Sports that combine large hip flexion with near-maximal knee extension seem to have a higher risk of this injury.
Less is known about this type of hamstring injury. What we do know is that recovery time for a stretch type hamstring injury is often longer than for the sprint type. This means that athletes return to their sport later. This makes the treatment of hamstring injuries complex and underlines the importance of a good guideline for diagnosis and rehabilitation.
Risk factors
Factors that increase the risk of a sprint-type hamstring injury:
Sports: Explosive sports with lots of acceleration and changes of direction. These are sports such as football and rugby. Classical sprinting also carries a high risk because of the high speeds that can be reached.
Level of sports practice: The higher the level, the higher the risk. This probably also has to do with athletic skills.
Age: Older athletes within this category are more at risk of injury.
Previous injuries: Those who have already had a hamstring injury are more likely to be injured again.
Complaints and symptoms
Sprint type hamstring injury
A sprint-type hamstring injury is often experienced as an acute, sudden pain at the back of the thigh. This usually occurs during a sprint or explosive movement. A sharp pain or even a kind of snap is often observed at the time of the injury.
Within hours, swelling and bruising may occur, indicating damage in the muscle. However, this may not always be the case because the hamstring and surrounding muscles have many different connective tissue layers. Often there are symptoms during normal walking and applying force against resistance gives recognisable pain.
Stretch type hamstring injury
In a stretch type hamstring injury, the pain usually occurs gradually or as a result of an extreme stretching movement as explained earlier. The pain is often less acute than with the sprint type, but can persist and worsen with many of the same movements.
Swelling and bruising are almost never present, The athlete does experience marked pain and limited range of motion when stretching the hip and fully extending the knee. Recovery often takes longer than with a sprint-type hamstring injury. For this reason, athletes may experience long-term restrictions in their sport, if at all possible. Proper rehabilitation is crucial to allow return to sport without increased risk of recurrence.
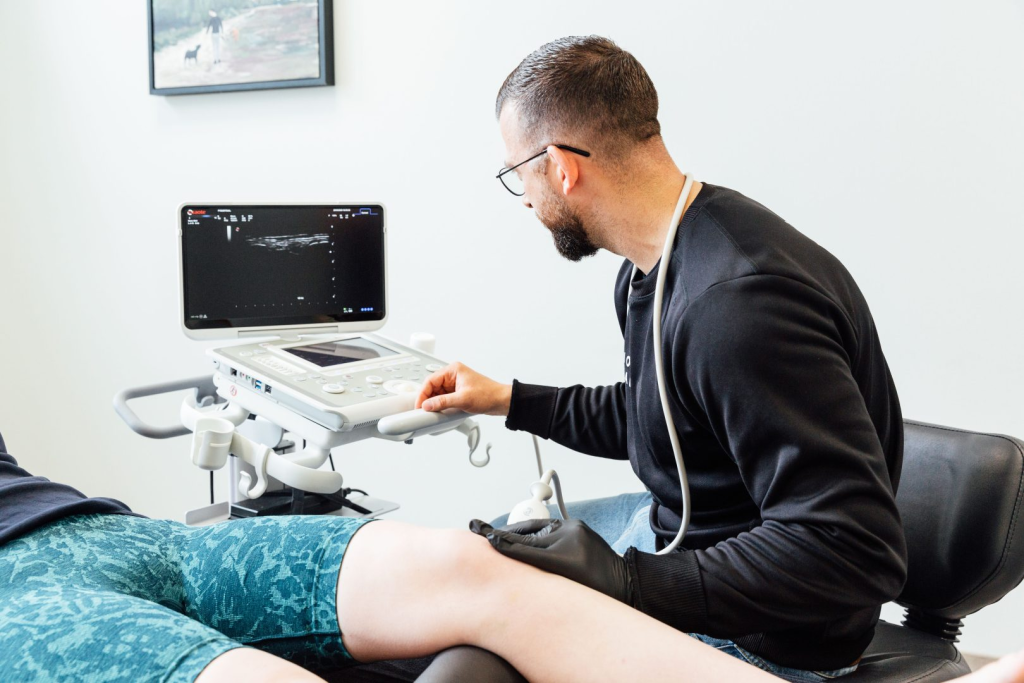
Diagnosis and examination
A proximal hamstring injury is difficult to map clearly. Traditional clinical tests using physical examination often provide an indication, but lack the precision to classify the exact location and severity of the injury. Ultrasound offers a quick and detailed complement. The advantages over an MRI may also be to assess the tendon dynamically.
The physical examination includes specific tests evaluating mainly strength and length tests. In addition, an easy way to provoke sensitivity around the tuber ischiadium (sitting bone) is by palpation.
An avulsion fracture of the proximal hamstring occurs when the tendon pulls on the bone with such force that a piece of bone of the tuber ischiadicum detaches. This is especially common in young athletes because their growth plates are not yet fully closed, making the bone more vulnerable than the tendon. In the case of a minimum displacement (<1-2 cm), a non-operative approach is usually chosen. Otherwise, surgery may be considered.
Treatment and prognosis
Treatment of a proximal hamstring injury focuses on load control and progressive strength training. The main interventions are:
Pain management and activity modification
It is important to avoid recognisable symptoms during the first phase of recovery. Especially a lot of stretching on the hamstring should be avoided. Total rest should be avoided but too much strain is pointless.
Eccentric and isometric training
Isometric exercises (e.g. single-leg bridge hold) can reduce pain and make the tendon more tolerant to strain again.
Eccentric loading such as nordic hamstring curls are used as a continuation of this isometric loading.
Progressive strength and stability training
Focus on hip-dominant exercises such as deadlifts and Romanian deadlifts for strength and control in the hamstring and gluteal region.
Gradual build-up to functional movements and sport-specific loading.
Return-to-sport criteria
Progressive build-up of explosive load, such as sprints and acceleration exercises.
The forecast of a proximal hamstring injury depends on the severity of the injury, the duration of symptoms and the effectiveness of rehabilitation. In general:
- Acute injuries (such as a mild tendon strain or minor damage) often recover within 6 to 12 weeks.
- Long-term tendonitis need a longer recovery period from 3 to 6 months, where consistent build-up of strength and load is essential.
- Partial or complete ruptures may have a recovery period of 6 months or more seize. Very rare with surgical intervention.
A good treatment plan with progressive loading and muscle-strengthening therapy increases the chances of full recovery and reduces the risk of recurrence. Factors such as age, activity level and previous injuries can influence the prognosis.
Possible other forms of complaints and diagnosis in proximal hamstring complaints
A bursa inflammation in this region (bursa ischiadica) can cause similar symptoms similar to a tendon injury of the proximal hamstring. This often results in a nagging pain in the buttock. The image of an ischiadica bursitis shows a large hypoechogenic area with an irregular outline. Deeper thrombosis may possibly also give symptoms of a typical hamstring injury. These symptoms cause a dull pain over the back of the thigh. Ultrasound examination may possibly signal deep venous thrombosis.
Do you recognise yourself in any of the above images? Then contact Fysio Fitaal in Tilburg. We are a modern Physiotherapy practice with a focus on sports physiotherapy and physiotherapy after surgery. Besides our commitment to your rehabilitation and recovery, we use innovative and measurable physiotherapy.
Related complaints

Hamstring
The hamstrings are a group of muscles at the back of your thigh. This muscle group...
Making an appointment at FysioFitaal
We work from multiple locations in Tilburg, always close by for professional and accessible physiotherapy. Fill in the contact form and we will contact you soon. Together, we will work on your recovery!